TCC Core
The AI-powered telemedicine platform
Eligible under KHTFV §3 (3) Telemedicine network structures
The hub-and-spoke model of TCC Core connects central tertiary care centers with smaller hospitals, practices, and care facilities. This creates a digital healthcare network that ensures quality across the board, improves care, and reduces the workload for medical staff.
Modular design + scalable networking + funding-eligible concept
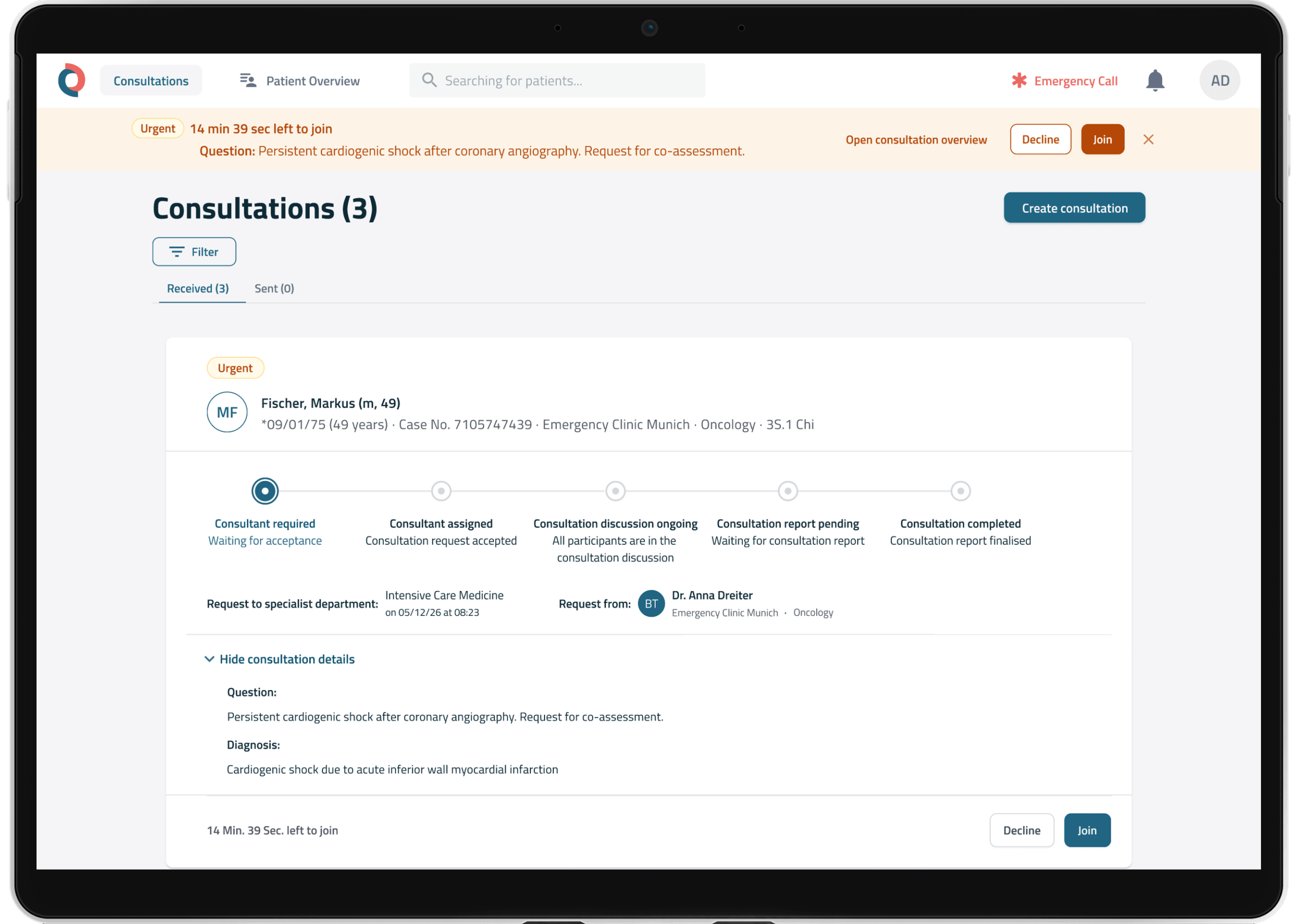
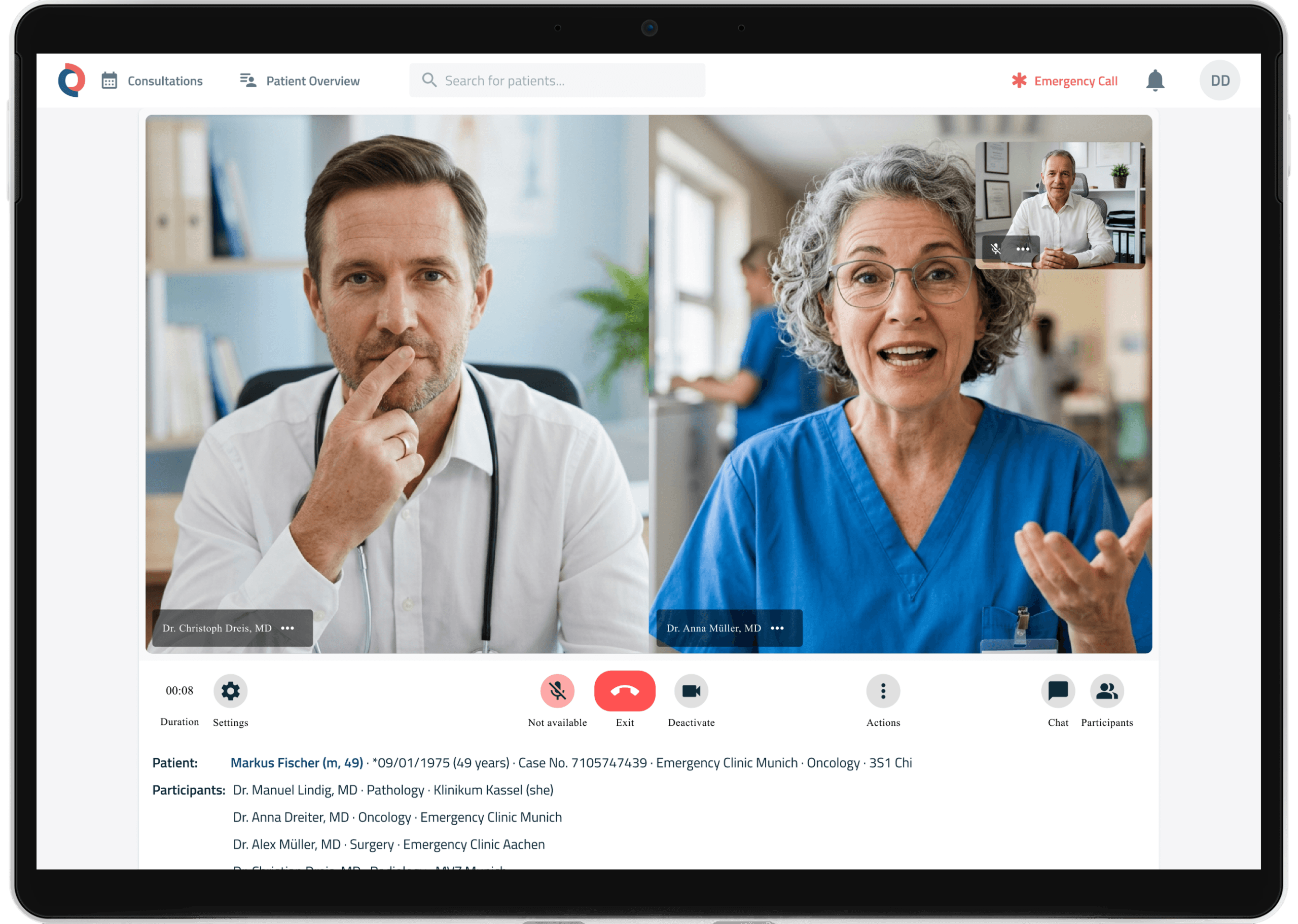
The TCC platform has a modular design, allowing various functionalities to be used after a one-time integration. This means that the platform can be flexibly adapted to specific requirements.
Services:
- modular, scalable platform with open interfaces
- display of real-time data & AI support
- interdisciplinary collaboration on a single platform
- Command Center function for hospital management
- eligible under KHTFV §3 (3) Telemedicine network structures
Modular and scalable design
TCC Core + Connect network module
TCC Core, in combination with the Connect network module, enables modern digital networking of medical facilities, including data exchange.
Cockpit module
The TCC Core Module Cockpit visualizes and synchronizes a detailed patient overview with patient data. It enables the integration of AI modules for prediction as well as intelligent data analysis. Using the patient dashboard and the Competence Center’s sorting function, patients can be sorted by vital signs, lab results, master data, or organ support data.
In the future, patients with significant changes can be intelligently highlighted using new prioritization scores such as the Telemonitoring Ranking Score and the Early Deterioration Score.
Predict module
The Predict module, in combination with the Cockpit module, supports decision-making in the treatment and prevention of medical conditions, such as acute kidney injury or sepsis.
Controlling module
The Controlling module collects all data relevant to capacity planning and displays it in intuitive dashboards, such as those for bed occupancy or length of stay.
Future module
Intelligent module
The Intelligent module analyzes data from medical facilities and enables efficient and sustainable management.
Future module
Radiology module
The Radiology module manages and synchronizes patient data from the radiology department.
Module under development
Testimonials
“This major project is an important milestone for KRH in its move towards modern digitalization and enables experts from all disciplines to be available around the clock and directly at every patient's bedside.”
PD Dr. Jan-Hinrich Baumert,
Medical Director of Intensive Care Medicine at KRH

“The establishment of digital cloud solutions and a TCC service for intensive care units relieves the burden on local IT, doctors, and nursing staff. This represents a concrete innovation in hospital operations.”
Rudolf Dück
CIO UKSH
Partner